Model
Model
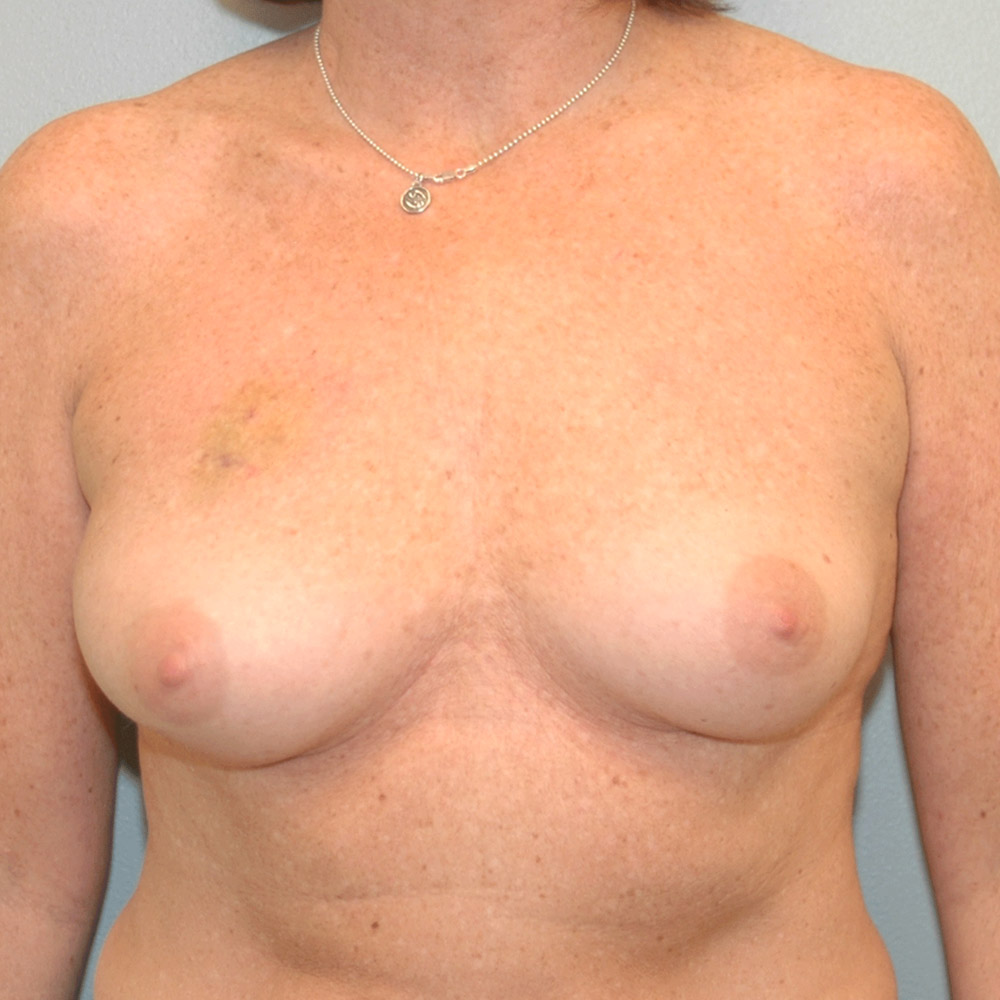
Breast Reconstruction in Portland & Lake Oswego
Dr. Elisa Burgess and her team are committed to providing exemplary breast cancer reconstruction in the most caring and compassionate manner. Breast cancer reconstruction is a specialized group of surgical procedures which recreate the breast, following a mastectomy or lumpectomy. Dr. Burgess guides her patients towards the best option for their specific situation, with optimal outcome. Reconstructed breasts will look different from your natural breast, but they can look very nice and natural in clothing.
Implant Reconstruction:
Tissue Expanders
During mastectomy, or a later date, tissue expanders can be placed above the muscle (prepectoral) or under the muscle (subpectoral). The prepectoral placement may decrease animation movement of the tissue expander when the pectoralis muscle is flexed, so this may look like a more natural reconstruction. The tissue expander is a temporary implant that contains a port within its shell. This port allows for adding more saline once the mastectomy incision has healed to fill the tissue expander. This process is known as expansion. Expansions start after surgery and occur every one to two weeks until you have reached your goal.
During a quick, in-office procedure, Dr. Burgess or her staff will use a very fine needle to place about 50mL of saline into the port of your tissue expander, through a numb area on your chest. The area may feel tight and uncomfortable that evening. Each patient has their own expansion schedule that can work around chemotherapy appointments, and their personal life. The number of required expansions is very patient-specific. Your final expanded volume depends on your individual goals and your anatomy. Once you have reached a volume that you and Dr. Burgess feel is acceptable, you will undergo a surgery to remove the expander and replace it with a silicone or saline implant.
Acellular Dermal Matrix (ADMs)
After mastectomy, the remaining tissue over the chest wall may be thin. An Acellular Dermal Matrix (ADM) is often a human cadaveric or porcine product that’s utilized at the time of tissue expander placement. It is possible that the expander or implant could be placed on top of the muscle. However, it would typically be wrapped in a large piece of ADM. If the reconstruction is partially under the muscle, the natural anatomy of the pectoralis muscle may not be adequate coverage for the implant. In this case, an ADM may be employed to provide lower pole for better support and coverage if partially under the muscle. The ADM is sewn into the pectoralis muscle, allowing for greater support in the lower breast pole, while supporting the tissue expander and eventually, the implant. It can provide a natural shape or “hang” to the breast. ADMs also support cellular growth and healing, while providing stabilization of the implant.
Resorbable Surgical Scaffolding Or Mesh (Internal Bra)
As an alternative to an ADM, an absorbable mesh can be used almost like an internal bra can offer crucial support for patients undergoing breast reconstruction, providing additional lift, shape, and long-term structural integrity. By using bioresorbable mesh materials like DuraSorb or GalaFLEX, the internal bra acts as an internal scaffold that gradually dissolves, allowing the body’s natural tissue to take over the role of support.
- DuraSorb: This bioresorbable, sterile monofilament mesh dissolves more quickly, offering initial support while enabling the formation of natural tissue in its place. Although FDA-approved for soft tissue support in reconstructive and cosmetic surgeries, its use in breast reconstruction is considered off-label.
- GalaFLEX: This bioresorbable, sterile monofilament knitted mesh dissolves more slowly, providing extended support as it integrates with the body’s tissue over time. It is FDA-approved for soft tissue reinforcement in plastic and reconstructive surgery, though its use in breast reconstruction is considered off-label.
These materials can be particularly beneficial for patients with thin tissue, those undergoing revision procedures, or those seeking added lift or support in their reconstruction while maintaining natural movement.
Direct To Implant
Direct-to-implant reconstruction surgeries are performed at the time of mastectomy. They require the general surgeon and the plastic surgeon working in sync for part of the same procedure. Patients who have sufficient breast skin remaining after mastectomy may be well suited for direct-to-implant breast reconstruction. While the direct-to-implant method avoids use of tissue expanders, secondary procedures may be preferred to improve symmetry or breast size. Unless the initial mastectomy was done using a nipple-sparing approach, most women proceed with nipple tattoo or reconstruction of the nipple and areola.

 Model
Model
Flap Reconstruction:
Latissimus Dorsi Flap
Another option for some is to reconstruct the breast using their own skin, tissue and latissimus muscle taken from the back and tunneling it to the breast area. This surgery is a favorable procedure for those who have undergone radiation and need fresh tissue to the chest. This is a major surgical procedure that can take 4-5 hours. Most women require several weeks off of work and should not work out vigorously for 8 weeks. Some patients require an expander for additional volume, which is replaced with a final implant once the process is complete. Patients can expect a scar on the mid-back/shoulder area.
Tram Flap
TRAM (transverse rectus abdominis muscle) flap is a major surgical procedure. It involves using your own abdominal skin, fat and muscle to create and contour one or both breasts but sometimes implants are also still necessary. This surgery can be upwards of 12 hours of surgical time and a 2-4 day hospital stay. The recovery from this surgery, as compared to the tissue expander procedure, is a greater length of time.
Diep Flap & Muscle Sparing Tram
The DIEP Flap and muscle sparing tram types of breast reconstruction uses your own skin and fat to recreate the breast from the abdominal area. In this microsurgical procedure, blood vessels known as the deep inferior epigastric perforators, (DIEP) along with skin and fat, are removed from the abdomen and relocated to the chest to create breasts. This type of flap surgery leaves the abdominal muscles intact. This surgery can be upwards of 12 hours of surgical time and a 2-4 day hospital stay. The recovery from this surgery, as compared to the tissue expander procedure, is a greater length of time. However, due to the complexity of this surgery, there are few facilities that offer the DIEP technique. Dr. Burgess does not routinely perform them but would be happy to refer you to a surgeon who does.

 Model
Model
Lumpectomy And Breast Reduction
Sometimes a breast reduction may be an option for larger breasted women who have been diagnosed with breast cancer. The mass is removed at the same time as the breast reduction. Many factors are considered, such as specific cancer diagnosis, stage, tumor location, breast size, treatment modalities and personal goals.
Following lumpectomy, a breast reduction will remove excess breast and fatty tissue in one or both breasts. This will make them smaller, lifted and more proportional to your body. Your size, anatomy and tumor location will dictate what type of surgical approach your plastic surgeon may use.
 Model
Model
All About the Implants
Choosing the right breast implant is an important part of your surgical journey. At Burgess Plastic Surgery, we offer four trusted brands— Natrelle, Mentor, Sientra, and Motiva—each with unique features to suit different needs and aesthetic goals. Below, you’ll find an overview of each implant option to help you make an informed decision with your surgeon.
Natrelle®
Offers both saline and silicone implants, including the highly cohesive Natrelle INSPIRA® collection.
Mentor®
Provides MemoryGel®, MemoryGel® Xtra, MemoryShape®, and saline implants.
Sientra®
Specializes in silicone gel implants, known for their high-strength cohesive gel and exclusive use by board-certified plastic surgeons.
Motiva®
Offers Ergonomix® and Round implants, known for their softer feel and innovative designs.

 Model
Model
The Refinements:
Fat Grafting
We perform fat grafting in conjunction with other methods of reconstruction. Dr. Burgess will remove fat from another part of your body (i.e. stomach or thighs) and place back into flatter areas of the reconstructed breasts to create better fullness and to fill indentations.
Nipple Reconstruction or 3D Nipple Tattoo
Once your breast reconstruction is complete, you may consider undergoing nipple reconstruction or 3D nipple tattoos. The majority of our patients now do the 3D nipple tattoo since it can look very natural and is easy to do. This usually occurs at least three months after your final implant placement or muscle flap surgery. However, nipple reconstruction may be done much later, depending on patient preference. Nipple reconstruction is a quick day surgery which uses your own tissue on the breast to create a nipple. The reconstructed nipple has projection, but no feeling or function. The areola is created by bringing in skin from another area of the body as a skin graft and then covering the nipple areolar complex with a protective dressing for about 5-6 days. Once this dressing is removed, care must be taken to not injure them. Patients should avoid vigorous exercise for about one month. Most patients do not require much time off of work, usually only a few days.
Surgery to Unaffected Breast
Some women chose to only have a mastectomy to the affected or cancerous breast. This is known as a one-sided or unilateral mastectomy. To create symmetry between the reconstructed breast and the natural breast, patients often require surgery to the unaffected side. The type of surgery is patient specific. Some smaller breasted women may require an augmentation, or implant to the natural breast, while some women may only need a breast lift. Others still may need a breast reduction to the non-cancerous breast if they are naturally very large breasted. Surgery to create symmetry is normally done at the time your final implant is placed to your reconstructed side, or after you have healed from your muscle flap surgery. With unilateral reconstruction there is no firm time frame for surgery to create symmetry.
The entire reconstruction process can take around one year to complete. Each patient has their own reconstruction timetable, with independent factors, such as chemotherapy, radiation or personal and family agendas that may affect surgery scheduling. Breast reconstruction is usually a staged process to allow for healing, settling of the new breasts or implants and mental adjustment to your new look. Because breast cancer reconstruction is an elective procedure, patients should be in good overall health.
Support
There are many support groups available to those with breast cancer, breast cancer survivors and their families. For more information, please click below.
Transformations That Speak Volumes
See What Our Patients Are Saying
Dr. Burgess and her professional staff are top notch. From the initial consultation to the final results, I couldn’t be more pleased
Dr. Burgess performed Ultherapy around my mouth and lips and within 3 weeks I felt firmer and my lips appeared to be ‘lifted’ and more shapely. Now at 2 months, I am enjoying a more defined lip line. The procedure was less painful than I expected and took less than 30 minutes.
I have visited Burgess Plastic Surgery several times for a variety of reasons. I have never had a bad experience. First of all, the clinic is always clean, warm, and inviting. The staff is friendly and helpful. They are eager to help and answer questions and make me feel safe and secure. Dr. Burgess is amazing! She always has the right ideas and I always walk away feeling beautiful without any pressure! I highly recommend this clinic!
I was really nervous about the whole process but the staff made me feel very comfortable with my procedure. She changed my life!
 Model
Model
Schedule A Consultation With Dr. Burgess.
If you have questions regarding reconstruction procedure options, do not hesitate any longer to schedule a consultation with Dr. Burgess. You can call 503-699-6464 and reach our office today. You can also submit an online contact form and we will get back to you at our earliest convenience.
Schedule a Consultation